 
I would like to go ahead with the laser surgery and decided to go with a different doctor after all. The doctor suggested I should see a neuro-ophthalmologist, even though he thought it is probably nothing serious and he said it is likely could not be fixed. The doctor said both eyes looked healthy and they constrict and dilate symmetrically in low and bright light condition.(to clarify : changing % of pupil surface is the same, even though they are different in size). 
I brought up the size difference in my pupils during my preop exam. I’ve had it probably for a year already.Recently I decided to do a PRK vision correction surgery. I noticed that my left pupil is larger than the right one. Horner’s syndrome is important to diagnosis, because it can indicate a lesion in the brain stem ( stroke), neck ( carotid artery dissection) or lung apex ( Pancoast’s tumor). Furthermore, there is usually an associated lid ptosis and facial hypohidrosis. 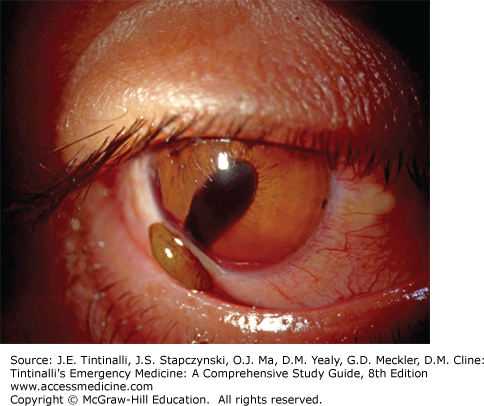
Horner’s syndrome causes unilateral miosis, and the affected abnormal pupil either does not dilate or has a delayed dilation in the dark. Physiologic anisocoria is mild (usually less than 0.5 mm difference in size between the pupils, and the amplitude of the difference does not vary greatly under dim or bright light conditions. If the smaller of the pupils is abnormal, a miosis, then the anisocoria will be more apparent (the affected pupil will be smaller) in dull ambient light conditions (a dark room), and less apparent (the pupils will be more equal) in bright light.Īlternatively, if the large pupil is the abnormal side, mydriasis, it will fail to contract in response to intense light.Ī unilateral miosis can be physiologic or can indicates a lesion affecting the sympathetic nerve fibers to the eye known as Horner’s syndrome. The first step in evaluating anisocoria is to determine which is the abnormal side – this can be accomplished by comparing the pupil sizes in response to bright light and dull ambient light: A prostaglandin analogue, such as travoprost, may be used if the intra-ocular pressure is elevated.Anisocoria – the pupils are unequal, is the the pupil too large, or is the left pupil too small? To subdue inflammation, topical corticosteroids can be used. If the pupil can be fully dilated during the treatment of iritis, the prognosis for recovery from synechia is good. Dilation of the pupil in an eye with synechia can cause the pupil to take an irregular, non-circular shape (dyscoria) as shown in the photograph. 
Mydriatic or cycloplegic agents, such as topical homatropine, which is similar in action to atropine, are useful in breaking and preventing the formation of posterior synechia by keeping the iris dilated and away from the crystalline lens. This blocked drainage raises the intraocular pressure. In posterior synechia, the iris adheres to the lens, blocking the flow of aqueous humor from the posterior chamber to the anterior chamber. Posterior synechia also cause glaucoma, but with a different mechanism. It is sometimes visible on careful examination but usually more easily through an ophthalmoscope or slit-lamp.Īnterior synechia causes closed angle glaucoma, which means that the iris closes the drainage way of aqueous humour which in turn raises the intraocular pressure. Synechiae can be caused by ocular trauma, iritis or iridocyclitis and may lead to certain types of glaucoma. Ocular synechia is an eye condition where the iris adheres to either the cornea (i.e. JSTOR ( October 2023) ( Learn how and when to remove this template message).Unsourced material may be challenged and removed. Please help improve this article by adding citations to reliable sources. This article needs additional citations for verification. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
